Answer Question Screen
- Clean multiple-choice interface with progress bar.
- Mark for review feature.
- Matches real test pacing.
Strike while the savings are hot! Use promo code FlashSale at checkout for 12% off any Exam Edge test or bundle. Hurry—the clock is ticking!

** All Prices are in US Dollars (USD) **
Understanding the exact breakdown of the DANB's Certified Dental Assistant test will help you know what to expect and how to most effectively prepare. The DANB's Certified Dental Assistant has multiple-choice questions . The exam will be broken down into the sections below:
| DANB's Certified Dental Assistant Exam Blueprint | |||
|---|---|---|---|
| Domain Name | % | Number of Questions |
|
| GC (120 Questions) | |||
| Collection and recording of clinical data | 10% | 5 | |
| Chairside dental procedures | 45% | 23 | |
| Chairside dental materials (preparation - manipulation - application) | 11% | 6 | |
| Lab materials and procedures | 4% | 2 | |
| Patient education and oral health management | 10% | 5 | |
| Prevention and management of emergencies | 14% | 7 | |
| Office management procedures | 6% | 3 | |
| RHS (100 Questions) | |||
| Expose and evaluate (intraoral - extraoral) | 37% | 19 | |
| Process | 16% | 8 | |
| Mount/label | 11% | 6 | |
| Radiation safety-patient | 24% | 12 | |
| Radiation safety-operator | 12% | 6 | |
| ICE (100 Questions) | |||
| Patient and dental healthcare worker education | 10% | 5 | |
| Prevent cross-contamination and disease transmission | 20% | 10 | |
| Maintain aseptic conditions | 10% | 5 | |
| Perform sterilization procedures | 15% | 8 | |
| Environmental asepsis | 15% | 8 | |
| Occupational safety | 30% | 15 | |
Everything you need to prepare with confidence—without wasting a minute.
Timed, No Time Limit, or Explanation mode.
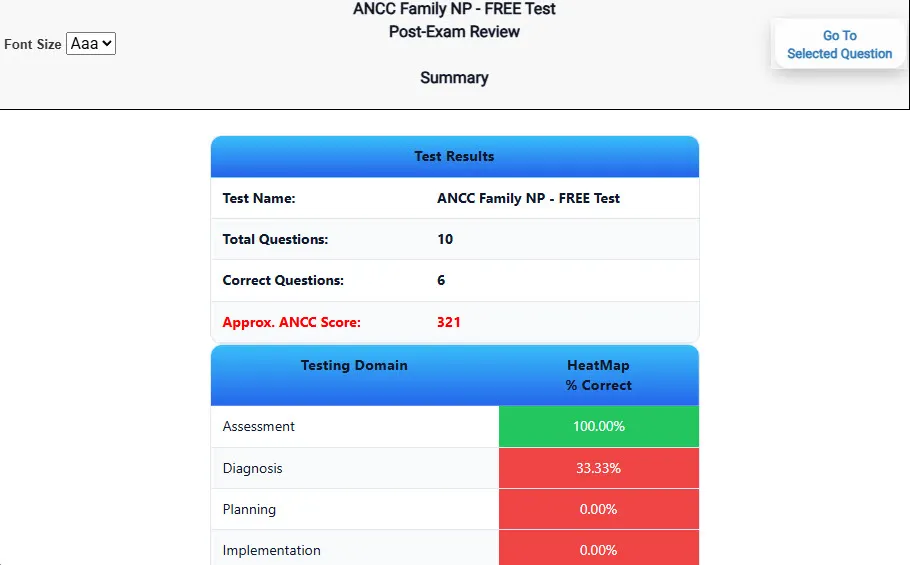
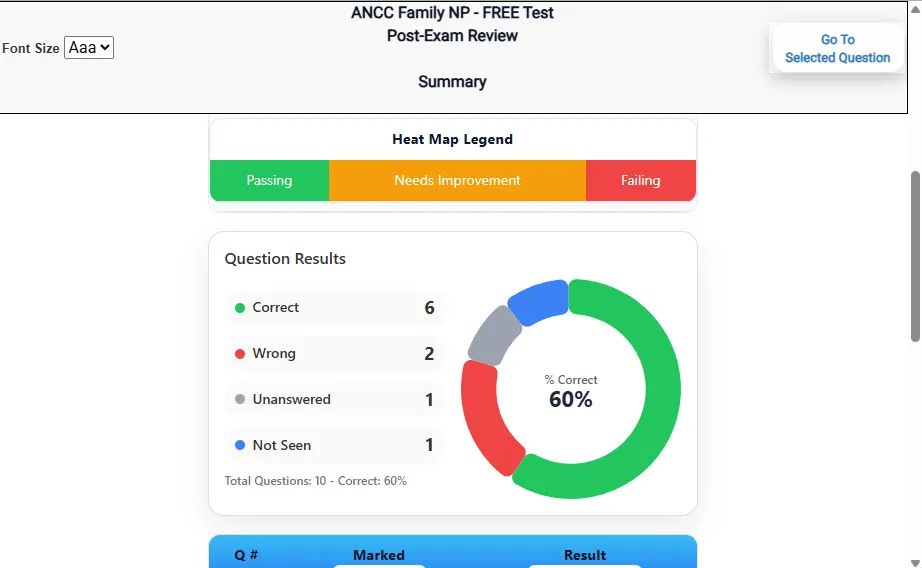
Heatmaps and scaled scores highlight weak areas.
Concise explanations emphasize key concepts.
Matches the feel of the actual exam environment.
Clean layout reduces cognitive load.
Web-based access 24/7 on any device.

Our practice tests are built specifically for the DANB's CDA exam — every question mirrors the real topics, format, and difficulty so you're studying exactly what matters.
We match the per-question time limits and pressure of the actual DANB's exam, so test day feels familiar and stress-free.
You'll have more than enough material to master every DANB's CDA concept — no repeats, no fluff.
Ordering 5 practice exams costs less than retaking the DANB's Certified Dental Assistant exam after a failure. One low fee could save you both time and money.
Need to step away mid-exam? Pick up right where you left off — with your remaining time intact.
See your raw score and an estimated DANB's Certified Dental Assistant score immediately after finishing each practice test.
Review correct and incorrect answers with clear, step-by-step explanations so you truly understand each topic.
We're fully accredited by the Better Business Bureau and uphold the highest standards of trust and transparency.
No software to install. Access your DANB's CDA practice exams 24/7 from any computer or mobile device.
Need extra help? Our specialized tutors are highly qualified and ready to support your DANB's exam prep.
Preparing for your upcoming DANB's Certified Dental Assistant (CDA) Certification Exam can feel overwhelming — but the right practice makes all the difference. Exam Edge gives you the tools, structure, and confidence to pass on your first try. Our online practice exams are built to match the real DANB's CDA exam in content, format, and difficulty.
These DANB's Certified Dental Assistant practice exams are designed to simulate the real testing experience by matching question types, timing, and difficulty level. This approach helps you get comfortable not just with the exam content, but also with the testing environment, so you walk into your exam day focused and confident.
“ Yesterday I passed my CDA test. Your test really helped me and I just wanted to say thank you.
“ I found the practice tests extremely helpful. I passed the DANB RHS exam and felt that the subject matter was thoroughly covered by your practice tests. The viewing of films and answering questions on them was especially helpful. Thank you very much for the assistance in preparing for the DANB RHS e ...
“ Easy to purchase & easily accessible. Great tool to use
Here is a list of alternative names used for this exam.